Abstract
Objective:
To examine the role of vestibular inputs on respiratory and oromotor systems in healthy preterm infants.
Study Design:
A total of 27 preterm infants were quasi-randomly assigned to either the VestibuGlide treatment or control groups. VestibuGlide infants were held in a developmentally supportive position, given a pacifier and received a series of vestibular stimuli, counterbalanced across rate and acceleration conditions, 15 min 3 times per day for 10 days. The control infants were also held in a developmentally supportive position, given a pacifier for 15 min 3 times per day for 10 days but did not receive the VestibuGlide stimulation.
Result:
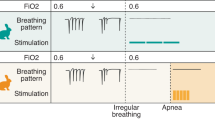
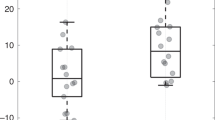
A multi-level regression model revealed that treatment infants increased their respiratory rate in response to vestibular stimulus, and that the highest level of vestibular acceleration delivered to the infants (0.51 ms−2) resulted in a significant increase in breaths per minute.
Conclusion:
Vestibular stimulation delivered to preterm infants before scheduled feeds effectively modulates respiratory rate and resets the respiratory central pattern generator.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Allin M, Matsumoto H, Santhouse AM, Nosarti C, AlAsady MH, Stewart AL et al. Cognitive and motor function and the size of the cerebellum in adolescents born very pre-term. Brain 2001; 124: 60–66.
Brown J, Minns RA . A Neurodevelopmental Approach to Specific Learning Disorders. Clinics in Developmental Medicine. MacKeith Press: London, 1999, pp 24–75.
Schaefer M, Hatcher RP, Barglow PD . Prematurity and infant stimulation: a review of research. Child Psychiatry Hum Dev 1980; 10: 199–212.
Barlow SM, Finan DS, Lee J, Chu S . Synthetic orocutaneous stimulation entrains preterm infants with feeding difficulties to suck. J Perinatol 2008; 28: 541–548.
Dieter JN, Emory EK . Supplemental stimulation of premature infants: a treatment model. J Pediatr Psychol 1997; 22: 281–295.
Blayney AW . Vestibular Disorders, 6th edn, vol. 6. Butterworth-Heinemann: Oxford, 1997, pp 1–29.
Nandi R, Luxon LM . Development and assessment of the vestibular system. Int J Audiol 2008; 47: 566–577.
Humphrey T . The Embryologic Differentiation of the Vestibular Nuclei in Man Correlated with Functional Development. Nippon-Hoechst: Tokyo, 1965.
Hooker D . The Prenatal Origins of Behavior. Hafner Publishing Company: New York, 1969.
Korner AF, Kraemer HC, Haffner ME, Cosper LM . Effects of waterbed flotation on premature infants: a pilot study. Pediatrics 1975; 56: 361–367.
Rice RD . The effects of the Rice infant sensorimotor stimulation treatment on the development of high-risk infants. Birth Defects Orig Artic Ser 1979; 15: 7–26.
Korner AF . Infant stimulation. Issues of theory and research. Clin Perinatol 1990; 17: 173–184.
Korner AF, Schneider P, Forrest T . Effects of vestibular-proprioceptive stimulation on the neurobehavioral development of preterm infants: a pilot study. Neuropediatrics 1983; 14: 170–175.
Neal MV . The relationship between a regimen of vestibular stimulation and developmental behavior of the small premature infant. Nurs Res Conf 1969; 5: 43–57.
Farrimond T . Sudden infant death syndrome and possible relation to vestibular function. Percept Mot Skills 1990; 71: 419–423.
Tuck SJ, Monin P, Duvivier C, May T, Vert P . Effect of a rocking bed on apnoea of prematurity. Arch Dis Child 1982; 57: 475–477.
Korner AF, Ruppel EM, Rho JM . Effects of water beds on the sleep and motility of theophylline-treated preterm infants. Pediatrics 1982; 70: 864–869.
Stradling JR, Chadwick GA, Quirk C, Phillips T . Respiratory inductance plethysmography: calibration techniques, their validation and the effects of posture. Bull Eur Physiopathol Respir 1985; 21: 317–324.
Boliek CA, Hixon TJ, Watson PJ, Morgan WJ . Vocalization and breathing during the first year of life. J Voice 1996; 10: 1–22.
Singer JD . Using SAS PROC MIXED to fit multilevel models, hierarchical models, and individual growth models. J Educ Behav Statist 1998; 23: 323–355.
Goldberg ME, Hudspeth AJ . The Vestibular System, 4th edn. McGraw-Hill: New York, 2000, pp 801–815.
Barlow SM, Estep M . Central pattern generation and the motor infrastructure for suck, respiration, and speech. J Commun Disord 2006; 39: 366–380.
Yates BJ, Miller AD . Physiological evidence that the vestibular system participates in autonomic and respiratory control. J Vestib Res 1998; 8: 17–25.
Finer NN, Higgins R, Kattwinkel J, Martin RJ . Summary proceedings from the apnea-of-prematurity group. Pediatrics 2006; 117: S47–S51.
Darnall RA, Ariagno RL, Kinney HC . The late preterm infant and the control of breathing, sleep, and brainstem development: a review. Clin Perinatol 2006; 33: 883–914; abstract x.
Acknowledgements
This study was supported by grants NIH R01 DC003311-08 (SMB), NIH P30 HD02528 and NIH P30 DC005803. The authors express gratitude to Douglas Kieweg, BS (Center for Biobehavioral Neuroscience of Communication Disorders) for software design, Jaehoon Lee, PhD, for statistical assistance, Joan Wang, MSEE, for computer engineering support, as well as the many families who participated in this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Zimmerman, E., Barlow, S. The effects of vestibular stimulation rate and magnitude of acceleration on central pattern generation for chest wall kinematics in preterm infants. J Perinatol 32, 614–620 (2012). https://doi.org/10.1038/jp.2011.177
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2011.177
Keywords
This article is cited by
-
Central not peripheral vestibular processing impairs gait coordination
Experimental Brain Research (2017)